Relieving Back Pain from Osteoporosis
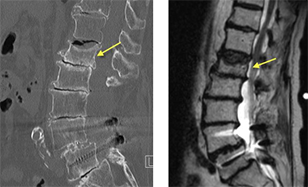
“Our involvement with osteoporosis is treating people who have osteoporotic compression fractures,” says Jack Jennings, MD, associate professor of radiology. “These are people who often have curved spines. Typically they’re in their sixth to eighth decade of life, more often female than male, with fractures (breaks) in their spines.”
In its most severe form, people develop a noticeable hump, sometimes called a “dowager’s hump.” The hump results from multiple bone breaks in the affected person’s backbone that cause the spine to collapse and a curvature to develop. The bone-thinning disease osteoporosis is often the underlying cause of this cascade of events.
Jennings is a musculoskeletal (MSK) radiologist. He’s a member of a group of specially trained radiologists at Mallinckrodt Institute of Radiology who diagnose conditions that affect the bones, joints and soft tissue in the extremities. But MSK radiologists also perform a variety of pain management procedures too, and osteoporotic bone fracture is one of the conditions they treat routinely.
Although conservative measures are always tried first, “people usually come to us after those have failed,” Jennings says. “They have tried letting the fracture heal on its own. They have tried braces. They may have even received an epidural or nerve block because they have more nerve pain than mechanical pain.”
To stabilize the fracture and reduce back pain, Jennings and his MSK peers inject cement through a ¼-inch-wide nick in the spine. The outpatient procedure is called a vertebroplasty, and it was first performed in Missouri by Mallinckrodt Institute radiologist, Louis Gilula.
“A vertebroplasty is a well-proven procedure with minimal risk that reduces back pain resulting from osteoporotic fractures,” says Jennings.
The patient receives conscious sedation but is awake enough to answer simple questions. They typically have no recall of the procedure later. “Most people feel better immediately with some experiencing procedural pain related to the needles.” Typically only one needle is needed.
“We do hundreds of these a year and have experience in doing complicated vertebroplasties, which bodes well for patients with less complicated cases.” Once you have an osteoporotic compression fracture you are likely to have another. That’s why any new pain should be investigated. “We want to treat these fractures before they completely collapse,” says Jennings.
For a consultation with Jennings or other MSK radiologists, please call 314-362-2825.





