She soon learned that her hip pain was being exacerbated by the fibroid’s position near her hip flexor muscle. It also was the cause of symptoms she had been dealing with for two years: heavy menstrual bleeding that left her incapacitated for a day or two each cycle, a bloated abdomen resulting from a bulky or enlarged uterus, and weight gain.
When Miller Erman visited her gynecologist to find out what treatments were available for uterine fibroids, she was stunned by his answer.
“He told me to get a hysterectomy,” she says. “As an athlete, that was a major, life-changing treatment. I was not willing to do that.”
A hysterectomy has been the standard of care for treating uterine fibroids for many years, and it continues to be the leading cause of the surgery in the U.S. Since patients seeking treatment are usually in their 40s or 50s, after their childbearing years are over, removing the uterus has been seen as a permanent solution to the problem.
Seeking a second opinion, Miller Erman was told she had another option: uterine fibroid embolization (UFE). The minimally invasive treatment relieves symptoms of uterine fibroids by cutting off their blood supply, causing them to shrink. It was the answer she was looking for, and it brought her to Sagine Berry-Tony, MD, assistant professor of radiology at MIR.
A Common Condition
“Uterine fibroids are extremely common,” Berry-Tony says. “They develop in over 95% of African American women and 80% of white women.”
Benign tumors made of muscle and connective tissue from the wall of the uterus, uterine fibroids can grow inside the uterus, within the organ’s wall or on its outer surface. They can be as small as an apple seed or grow to the size of a grapefruit or even larger. The reason uterine fibroids develop is unknown, but there is a proven connection between fibroids and the level of hormones in a woman’s body, because they grow during childbearing years and shrink during menopause. Some women with uterine fibroids have no symptoms and never know they have them. Others develop symptoms so severe they become life limiting.

“Some women experience such excessive bleeding during their periods that they have to change their pads several times an hour, sit on a towel or change their bedsheets daily,” says Steven C. Sauk, MD, chief of interventional radiology. “They can experience frequent urination, constipation, bloating, back and leg pain, cramps — a host of symptoms that are different for each woman.”
According to Berry-Tony, women often tolerate the symptoms and adjust their lifestyle, thinking that what they are experiencing is normal.
“Even going back as far as high school, women talk about having to stay home from school when their period came because the bleeding was so excessive. No one told them that’s not normal. It’s not until later in life they are diagnosed with uterine fibroids,” she says. “And there are women for whom the symptoms develop so gradually they don’t realize the adjustments they are making until they become intolerable.”
Helena Cody-Perry, 52, had been dealing with symptoms she thought were related to menopause. Once she was diagnosed with uterine fibroids, she grappled with the decision of whether to have a hysterectomy or undergo UFE.
“I was experiencing heavy bleeding, I gained weight, I had headaches, I was moody, I was tired all the time and my blood pressure was high, sometimes 150/100. I was a mess,” she says. “I had a lot of people tell me to have a hysterectomy. They reasoned that my having the surgery would be a permanent solution. They believed if I had a UFE, there was a good chance of even more fibroids growing back.”
Uterine fibroids occur in over 95% of African American women and 80% of white women.
Cody-Perry took about three months to consider her options. A conversation with Berry-Tony helped her decide on having a UFE.
“She explained the process, that it was outpatient surgery, and I would recover much more quickly than if I had a hysterectomy,” she says. “And she told me a hysterectomy was always an option if I wasn’t pleased with the outcome of the UFE procedure.”
New Standard of Care
A growing number of women regard a hysterectomy as too invasive a procedure. And some don’t want to lose a part of themselves that defines them as a person. UFE’s minimally invasive approach eliminates both of those concerns.
“The uterine arteries supply blood to the fibroids, and estrogen, the hormone that influences fibroids’ growth, is in the bloodstream,” Berry-Tony explains. “UFE cuts off the blood supply to the fibroids.”
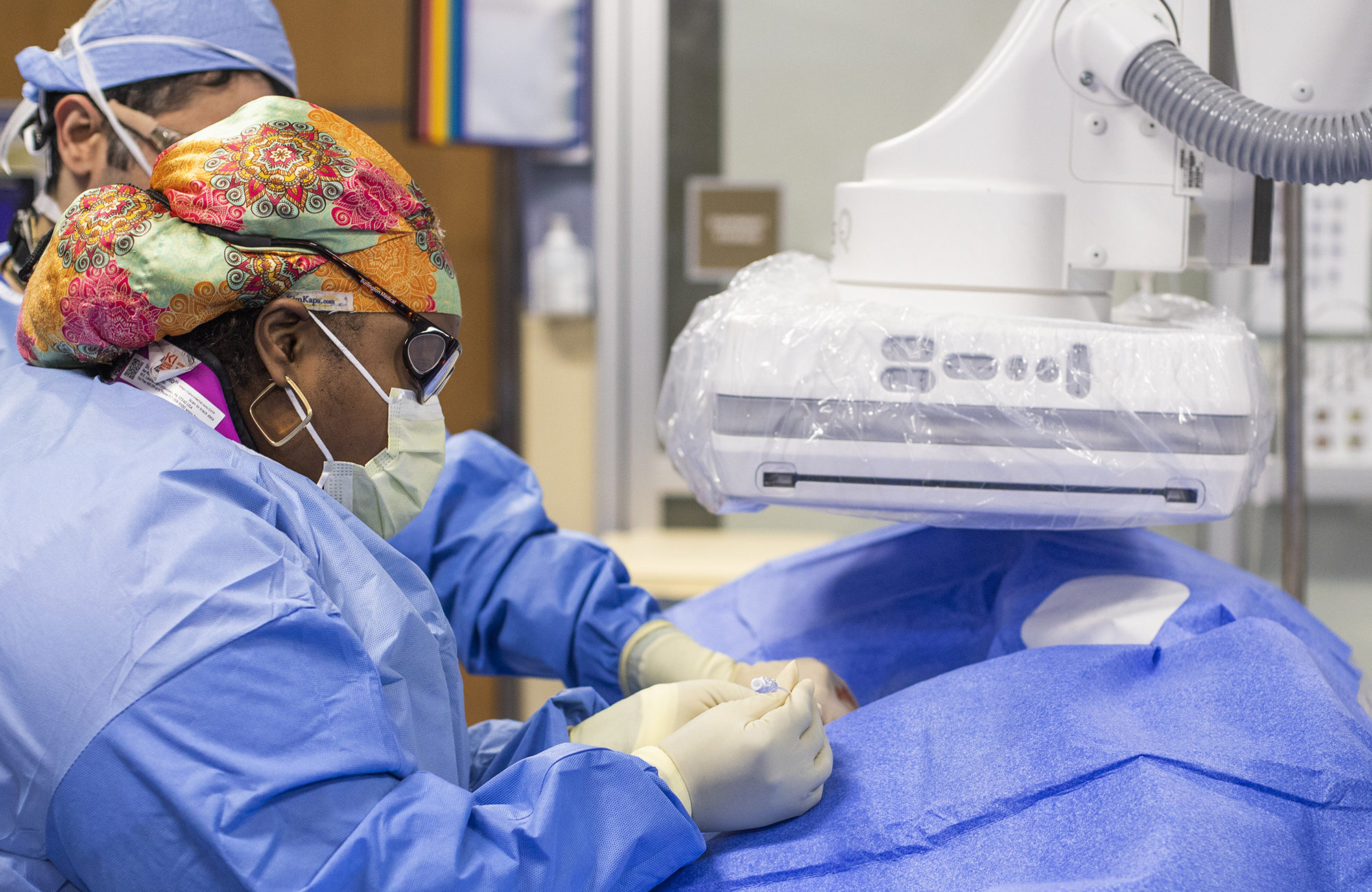
During the UFE procedure, a small catheter is inserted through a blood vessel in the patient’s wrist or groin and guided by X-ray to the right and left uterine arteries. Once the catheter is positioned, tiny particles are injected into each artery to stop the blood flow to the fibroids. Without a blood supply delivering oxygen and nutrients, the fibroids shrink, and over time patients’ symptoms subside.
“You can compare the particles to how sand is distributed in a river. The sand is carried downstream to an endpoint. In the case of UFE particles, that endpoint is all the capillaries supplying blood to the uterus and the fibroids,” Sauk says.
“Interventional radiologists at MIR have been performing UFEs since 2009,” he says, “at a time when UFE was still considered an ‘experimental’ procedure. That has given us significant experience in what is becoming the new standard of care for uterine fibroids.”

Most women with uterine fibroids are eligible to undergo a UFE. Prior to the procedure, the patient has an MRI to establish a definitive diagnosis of uterine fibroids and determine their location. Halfway through the MRI, a contrast dye is injected to trace blood flow, which includes the flow to the uterine fibroids. If the fibroids are responsive and active, they will “light up” on the scan.
“There are some women who have fibroids that aren’t using a blood supply,” Berry-Tony says. “This can result from fibroids getting so large that they begin degenerating on their own. Since UFE’s goal is to stop blood flow, these patients are referred for optional treatments of their symptoms.”
Once the procedure is completed, most patients are discharged within a few hours. They are provided with appropriate medication to manage any pain and instructions on what to do if they experience any problems. Brittany Schmitt is the clinical nurse coordinator who serves as the go-between for patients and their interventional radiologists, and for the radiologists and gynecologists. “Before the procedure, I reassure them that the symptoms they are experiencing are not normal, and I educate them on what will be involved in their treatment.
“I call patients two or three times the week after their procedures,” Schmitt says. “I make sure they are comfortable and troubleshoot any symptoms, giving suggestions about what they can do at home to help themselves. And I relay any concerns they may have to the physicians. I serve as their advocate.” She continues to follow up at one-month, three-month and six-month intervals.
Symptoms should get progressively better until patients reach the year mark. That becomes their new baseline.
Berry-Tony emphasizes that UFE does not remove uterine fibroids. They remain in the uterus, but without a blood supply, they shrink over time. Since most patients are in their 40s and 50s, the procedure acts as a bridge to menopause, when hormones drop low enough to prevent new fibroids from forming.
“After the procedure, we tell patients it will be about three period cycles before they first start noticing a decrease in their symptoms. And the symptoms should get progressively better until patients reach the year mark. That becomes their new baseline,” she says. “If after one-year post-embolization the fibroids have decreased in size by 50%, that should be enough to stop symptoms.”
Least Likely to Seek Treatment
Although uterine fibroids occur most frequently in Black women, they are the group least likely to seek treatment, Berry-Tony says. “For good cause, they have a distrust of the medical community and undergoing major surgeries such as a hysterectomy. They don’t believe they will be heard by their physicians, and their concern about a major complication developing while they are under anesthesia outweighs any relief they may have for their symptoms.”

She stresses that UFE can alleviate much of that reluctance. “Patients are under conscious sedation, they are breathing on their own, they can talk to me, I can talk to them. The procedure itself is not painful,” she says. “Afterward, patients are given specific instructions on what to do next and when, how to manage their pain and how to contact us with questions. It is a transparent procedure that can allay any fears patients may have.”
Following her procedure, Miller Erman experienced no pain or discomfort. “I was given pain pills, but I didn’t need to take them,” she says. “I was instructed to stay home for five days, which I did, but it was unnecessary — I was running again on day 6.” Although she says she can still feel the fibroid when she runs, it is not painful. All of her symptoms are gone, and she is back to training 14 hours a week so she can compete in half-marathons and duathlons.
Cody-Perry felt so good after UFE that she returned to work within two days. “I didn’t have any pain. I didn’t even have to sit down the whole time I was at work,” she says. “My symptoms subsided quickly: I no longer had heavy bleeding, my headaches stopped, I was able to exercise and lose weight, and my blood pressure is under control. It was a great experience.
“As a matter of fact, I was just talking to someone who is going through the same thing I did. I told her about my UFE procedure — and I told her that a hysterectomy was not her only option.”
Published in Focal Spot Spring/Summer 2023 Issue