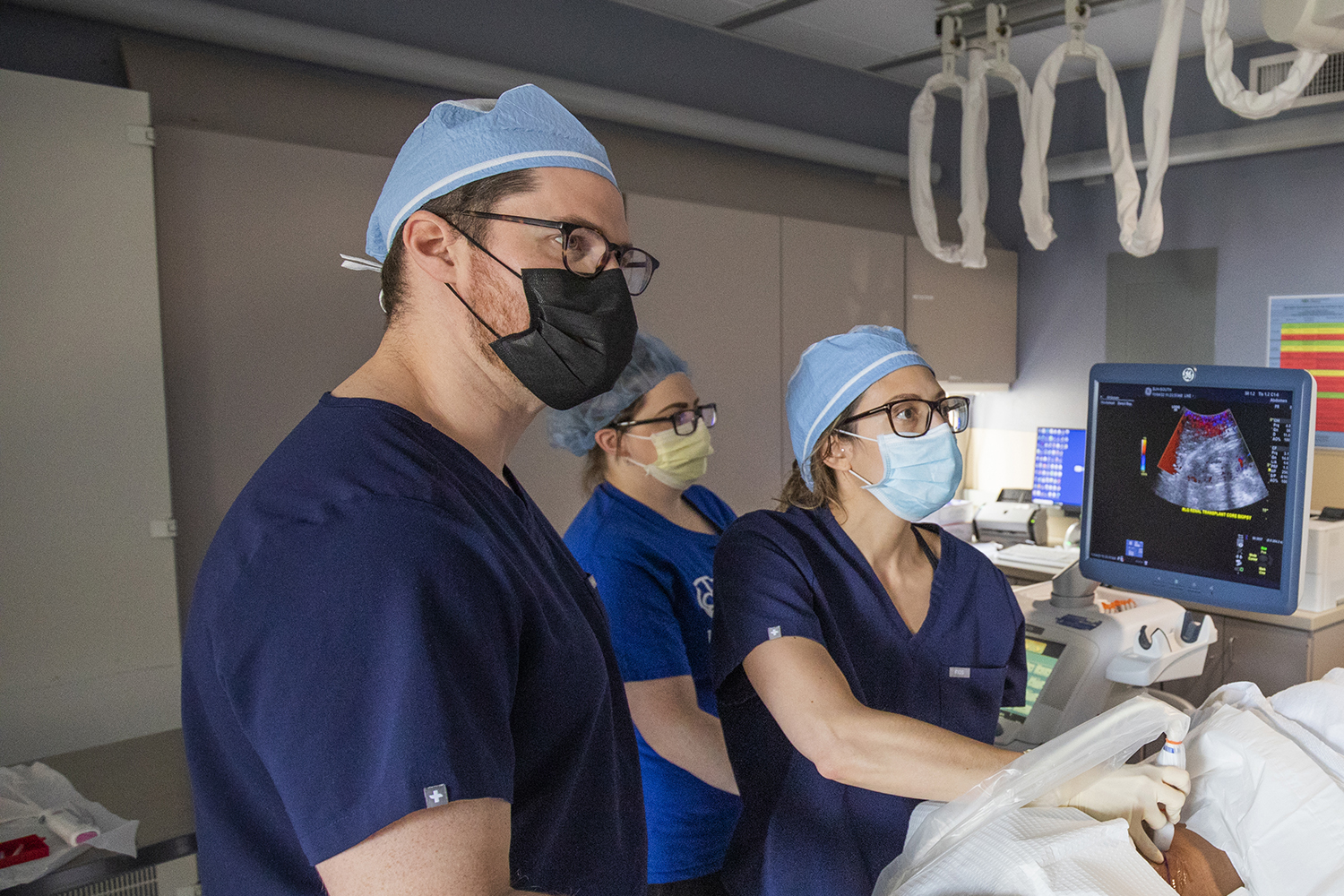
A new service line dedicated exclusively to deep-tissue biopsies is enabling a team of abdominal radiologists at MIR to provide more cohesive, comprehensive and consensus-based care for biopsy patients.
“The new dedicated service line has made the experience more pleasant for patients and the process go a lot more smoothly,” says Vincent M. Mellnick, MD, chief of abdominal imaging. The addition of staff, use of sedation for procedures and a dedicated recovery space have ultimately resulted in safer, more robust patient care.
Previously, biopsies were performed as part of normal diagnostic duties and based on modality. For example, an abdominal radiologist on the CT service would perform any CT-guided biopsies in between reading all the CT scans for that day. “There were a lot of inherent distractions associated with that method,” says Mellnick, associate professor of radiology. Pre-procedural assessment and post-biopsy monitoring also varied by modality and location.
“We determined that we needed a more organized and formal structure in which to assess, monitor and recover patients in a way that did not rely on the availability and attention of a person who was being pulled in multiple directions at the same time,” says Benjamin S. Strnad, MD, assistant professor of radiology. Strnad spearheaded the effort to launch the new service and coordinated key elements with radiology nursing leadership at Barnes-Jewish Hospital during the summer of 2020, when a reduced patient load provided time to strategize.
The new service line that emerged includes eight abdominal radiologists who all rotate on the service. They handle only deep-tissue biopsies of all modalities on the day they are on service and are responsive to any issues during recovery. Recovery is now standardized and occurs in dedicated post-procedural monitoring areas, such as the interventional radiology holding area or the surgical post-anesthesia care unit (PACU). The standard use of intraprocedural nurse monitoring and recovery has also enabled the service to routinely offer conscious sedation.
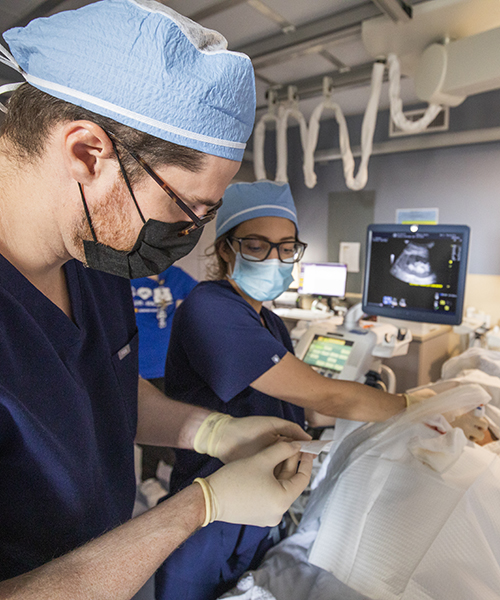
Two biopsy nurse coordinators were added to the service to facilitate screening of deep-tissue biopsy patients for risk factors and to facilitate medical optimization of higher-risk patients. Two physician assistants joined the service as well and alternate overseeing the daily logistics of the service, including the screening and initial work-up of any inpatient biopsies. They also act as the biopsy team’s point person if concerns about complications, particularly internal bleeding, arise during recovery.
The new service line’s team has significantly increased communication among its members, who often review biopsy requests together. “If someone has experience with a particularly challenging or unusual biopsy, they’ll chime in and say, ‘I know how to do this. You can schedule it with me’ or ‘I don’t think we should perform this biopsy and here’s why,’” Strnad says. “That consensus approach was not routine prior to this group being formed.”
As a result of this team approach, MIR now has the capacity to perform more ambitious biopsies, Strnad says. “We have a greater pool of knowledge and a much more structured and safer environment than we had before.”
Published in Focal Spot Fall/Winter 2022 Issue